Know your Injuries – Part 9: Shin Splints

Dr Meenakshi presents explains how to manage shin splints in Part 9 of her Sports Injury Management Series.
Shin Splints may be defined as pain in the lower leg caused by exercise or any sports activity. The most common cause is the media tibia stress syndrome or MTSS. It is an overuse condition that develops gradually over many days after a single excessive or intense training session.
Other shin conditions that may cause the symptoms include muscle strain, tendinopathy (microtears in the tendon), tibial stress fracture or a compartment syndrome (caused by lack of blood and oxygen to the leg muscles during exercise).

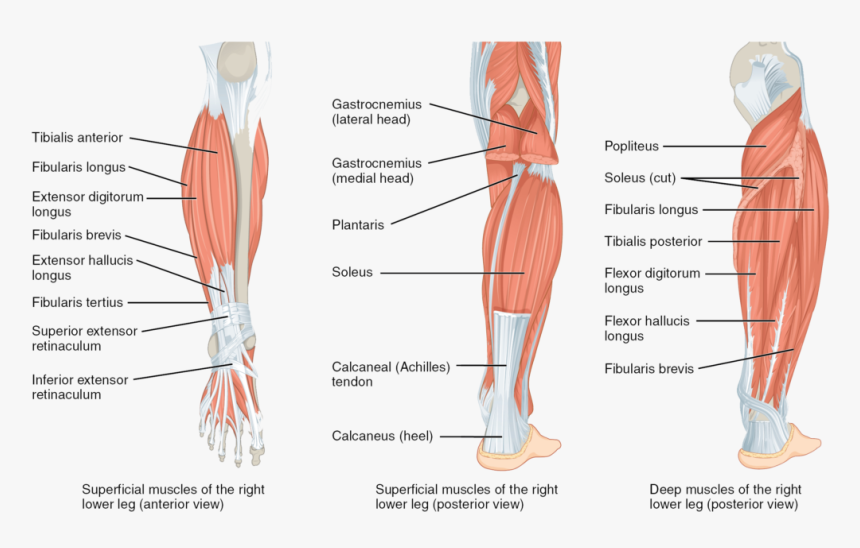
The tibia is the larger of the two bones in the lower leg – that is between the knee and ankle joints. Medial refers to the inner region of the tibia (the most common site for MTSS). Leg muscles, tendons and the bone covering are also involved.
Meenakshi breaks down her explanation in terms of –
- symptoms,
- causes,
- prevention,
- first aid,
- basic rehab movements
Symptoms
Signs include –
- Pain, dull ache or tenderness and sometimes swelling or redness in the medial, posterior or anterior region of the lower leg
- The pain may come and go as activity continues.
Causes
The condition is exercise or activity induced though the specific cause is difficult to pinpoint.
It may be periostitis (inflammation of the outer layer of the bone), myositis (inflammation f the muscles) or tendinitis (inflammation of the muscle – tendon complex) or a permutation and combination of two of these three. Faulty foot mechanics also can contribute to the injury.
It is pertinent to note that the risk of hamstring injury increases with –
- Sports involving extensive amounts of running, jumping activities – e.g. running, sprinting, basketball, football, gymnastics or figure skating.
- A novice who trains too hard and too long – it is common to see beginners in running getting these injuries!
- Cross-training or training which requires switching from one type of sport to another – e.g., triathlon
- High impact aerobics
- Running or training with ill-fitting or work out shoes
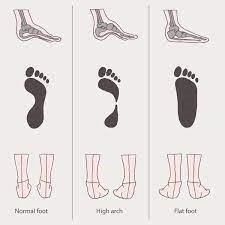
Foot arches that are pronated (flat) or supinated (high) or muscle imbalance in the leg muscles.
Prevention
Prevention is better than cure! The precautions to be taken are common to all sports and exercise injuries. But it is worth reminding the reader!
- Stretch and strengthen the lower leg muscles. Stretch before and after running
- Avoid hard and uneven surfaces
- Warm up adequately
- Avoid overtraining
- Wear proper shoes – high socks / stockings that support the lower leg muscles will also help
- Consider activities like swimming and cycling that have less impact on the shins.
First Aid
Follow the P.R.I.C.E. drill –
- Protect the injured part, not allowing any further damage.
- Rest the injured part.
- Apply ice or cold treatment for 15-20 minutes.
- Compression: use of mild to moderate pressure to the injured area with bandages / crepe bandages is advisable.
Current international standards have replaced P.R.I.C.E. with P.O.L.I.C.E.
- P – Protection of injured part
- O/L – Application of Optimal load (local injury factors) / Training load
- C.E. – as mentioned earlier (ice + compression+ elevation)
Follow up on First Aid
- Use ice massage. Massage the area in circular fashion for about 15 minutes three or four times daily.
- After about two days, apply heat through a hot water bag or infra-red lamp, or hot water soaks.
- Regular oil massage of the painful area will increase circulation and provide relief.
- Stop the activity that induced the shin splints in the first place.
- Your doctor ay recommend special shoes in case the splints are caused by flat or high arches of your feet.
- When ready to resume your normal sporting activity, ice the area for 5 to 10 minutes before warm up and after cool down.
Nutrition plays a big role in the recovery process and the injured person must consult a certified sports nutritionist.
Exercises to prevent injuries and strengthen the hamstrings
Dr Meenakshi (P. T.) recommends these rehab exercises to help recover from hamstring injuries. Watch her demonstrate these exercises.
A good stretching routine combined with strengthening exercises can be started after the pain and inflammation are no more. Calf raises (ankle joint plantar flexions) and shin flexions (ankle joint dorsiflexions) are highly recommended exercises. The stretches can be repeated several times a day, in fact.
Physical therapy may be advised in cases where pain and inflammation continue even after two to three weeks.
See your physiotherapist if your symptoms persist over 10 days or pain worsens despite treatment.
